Avoiding the Pitfalls in CPR/DNR Decision Making
September 6, 2010 by Viki Kind
Filed under Ask Viki, Newsletter
Avoiding the Pitfalls in CPR/DNR Decision Making
Educational Objectives:
Examine the obstacles to good DNR decision making.
Discuss what is CPR and the perceived vs. actual chance for success.
Demonstrate best practices for communicating about CPR.
Consider how the signing of the DNR is just one component of
end-of-life care.
Background:
Older adults and their loved ones are being asked to make difficult end-of-life choices about CPR (cardiopulmonary resuscitation) and its refusal, DNR (do not resuscitate). These decisions are fraught with emotional angst and misinformation. In the past, we only used CPR on patients who were having a heart attack and who might benefit from receiving CPR. Now we use it for everyone, including those in a terminal state, whether it will work or not.
One of the complicating factors is that CPR used to be very simple to understand. Now, the general public doesn’t realize that when the doctor says CPR, she is including medications, intubation and ventilator support. A common misunderstanding occurs when people are given the misleading choice of a “chemical code only.” As nurses and doctors will tell you, if the doctor gives the medicine but doesn’t do the chest compressions to move the blood around, the medicine will not circulate in the body. Without circulation, the medicine can not do its job.
Another factor is that the decision about CPR has inappropriately become an indicator of a person’s complete end-of-life wishes—but the decision about CPR should be only one part of the treatment plan. A patient may want chemotherapy, surgery, radiation therapy or other kinds of aggressive treatments and still may want to be a DNR. Or the person may not want other medical treatments but still want to receive CPR. These are all separate decisions and any combination is possible.
One positive change is that the language of DNR has been modified to “do not attempt resuscitation” (DNAR) or “allow natural death” (AND). Both of these help to clarify the confusion. Do not attempt resuscitation truthfully explains that just because CPR is attempted, doesn’t mean it will work. If you ask healthcare professionals, “How many of you would like to die by CPR?” No one ever, ever raises a hand. What they know, but don’t always share with their patients, is that the chance of CPR working is minimal, sometimes even 0 percent. On television shows like ER, CPR brings the patient back to life about 75 percent of the time (Diem, Lantos and Tulsky 1996), when in real life it only works, at best, 17 percent of the time on healthy patients (Peberdy, et al. 2003). In many real-life situations, the chance of success is zero.
William J. Ehlenbach, MD, lead author of a study of CPR in the elderly, published in the New England Journal of Medicine in 2009, explains, “CPR has the highest likelihood of success when the heart is the reason, as in an ongoing heart attack or a heart rhythm disturbance. If you’re doing well otherwise, CPR will often be successful. But, if you’re in the ICU [intensive care unit] with a serious infection and multiple organ failure, it’s unlikely that CPR will save you” (quote from Gordon 2009; study published by Ehlenbach et al. 2009).
The newest term, allow natural death or AND, is a more gentle way of saying do not resuscitate. Instead of stating what won’t be done for the patient, the doctor is offering to allow the patient a peaceful, natural death and will not attempt resuscitation. Because the CPR/DNR decision is about more than medicine, it frames the dying experience for the patient and the loved ones. For those who are making the CPR/DNR decision, it is important to balance the chances of CPR working and bringing the person back in a good condition with the desire for a good, peaceful and dignified death. This is why healthcare professionals wouldn’t want to die by CPR; there is nothing peaceful or dignified about this type of death.
Case study 1:
Mr. Jackson is a 67 year old gentleman who has end-stage Alzheimer’s, is unable to eat and recently had a feeding tube placed. The patient does not have an advance directive and never told his kids what he would want done and unfortunately, his doctor didn’t ask about his CPR wishes when he was in the early stages of the disease. The physician is now asking, “Would he want CPR?” His adult children have been through a lot over the past years and are overwhelmed by the question. The thoughts running their minds are, “Is it time? Are we giving up? I don’t want to make this choice but I can’t stand watching him suffer any longer. If I make this decision, does that mean I have lost my faith?”
How can the healthcare team help guide the adult children through this decision making process? What are the underlying issues that will make the decision more difficult to make? What statistical information might make the decision easier? What grief support can the healthcare team provide to ease the process?
Discussion – Mr. Jackson:
How can we as aging professionals help those we serve as they struggle with these difficult decisions? One of my roles as a bioethicist is to assist families, like Mr. Jackson’s, who are making the difficult decisions. I am not there to tell the family or healthcare team what to do, but to help those involved to think through the issues so they can make a more informed decision. It is important during these conversations that we keep the patient’s wishes and needs at the forefront.
When working with Mr. Jackson’s son and daughter, I would make sure they are educated about CPR. Hopefully, Mr. Jackson’s doctors will not have eroded the trust and created a confrontational relationship by pushing for the DNR. I would need to be patient as these end-of-life conversations are a process, not a one-time event.
I would make sure Mr. Jackson’s children understand the possible outcomes of CPR. He may survive CPR but never be able to leave the hospital or he may be hooked up to ventilators for the rest of his life. Research has found if CPR is able to bring a patient back to life, the chance of the person going home with good brain function is about 7 percent (Kaldjian, et al. 2009). And in Mr. Jackson’s compromised condition, his chances are even lower. The typical success rate of CPR will depend on the health of the patient, the patient’s age, how quickly the CPR was begun and other medical factors.
Next, I would make sure that the family understood what can happen during CPR. Mr. Jackson may be brought back to life but in a worse condition than before, both mentally and physically. There is a chance of broken ribs, a collapsed lung, damage to the windpipe, and the longer he isn’t able to breathe, the greater the chance for brain damage.
Once the family understands the likely chance of CPR working and what kind of outcomes might be expected, I would then point out that by discussing that by choosing CPR, Mr. Jackson may not have the opportunity for a peaceful and meaningful death experience. I would ask his children, “When your father pictured the last minutes of his life, did he see strangers straddling him on a bed, pushing on his chest, with his family waiting outside his door? Or would your father want his family and friends gathered around his bedside, with words of love being expressed, music being played or prayers being said?” By asking these important questions, I am helping to contextualize the medical choices by explaining what it will be like for their father to experience CPR versus a more peaceful death.
Another common issue I may have to address is to relieve the guilt and angst of those making these difficult decisions. One gift I may be able to give Mr. Jackson’s children is to help them understand that it not really their decision. It is the patient’s decision. I would explain that as the decision makers, they are supposed to consider all that they know about their dad, what he has told them in the past, what his values are, and what would be important to him. Using this information, they should do their best to make the decision they think their father would make.
I would gently ask, “What would your dad be telling us if he were able to understand what has happened? What would your dad say about wanting CPR?” And then I would be quiet and let them sit with the question. In most situations, the family will know the answer but it will be painful for them to verbalize the choice. I would then acknowledge how loving and courageous they are to honor their father’s wishes. No matter what decisions are made, it will be important that this family receive emotional and spiritual support as they struggle with these issues.
Case Study 2:
Mrs. Garcia is an 83 year old woman who has multiple sclerosis. Her advance directive states that she does not want CPR. Her multiple sclerosis has developed to the stage where she has lost the capacity to speak for herself. Her husband is her decision maker and caregiver and he knows her wishes. Last week, Mrs. Garcia suffered a heart attack and is now in the ICU. This morning she coded and was brought back to life by CPR. Her husband has just been called to come to the hospital and was told that his wife survived CPR but her condition is deteriorating. What went wrong? Why wasn’t her DNR honored? What is Mrs. Garcia’s expected outcome after receiving CPR?
Discussion – Mrs. Garcia
What went wrong?
Unfortunately, this scenario happens more often than it should. When Mr. Garcia got the call about his wife, he was shocked and angered. How could this happen?
There are a few possibilities. Some doctors won’t agree to a DNR because of moral opposition and therefore won’t write or respect a DNR. While doctors are allowed to live by their morals and to refuse to participate in acts that go against their values, they are still obligated to let patients know about valid medical options and then let the patient or decision-maker decide. If the doctor is unwilling to do this, then the doctor should help the patient to find another doctor who is willing to talk about the DNR option. If the patient, family or someone from the healthcare team is worried about the patient’s rights being violated, he or she should call for a bioethics consult from the hospital’s bioethics committee.
Another possibility is that the DNR request from her Advance Directive was not transferred onto her hospital chart. If the DNR is not on the chart, it doesn’t exist. Whether you are the patient, the loved one or someone working with the family, make sure you go over the patient’s Advance Directive and other healthcare wishes with the doctor and make sure they are documented.
A final possibility is that medical miscommunication occurred. Perhaps the advance directive wasn’t sent up from the emergency room, the team couldn’t find the DNR, no one took the time to look for it, the on-call physician wasn’t familiar with the patient or numerous other mishaps. As much as the public would like medicine to be perfect, healthcare is significantly flawed and human.
What should happen next?
The first step will be to make sure the DNR order is written immediately. I would hope that apologies would come next. Administration, risk management and other hospital staff will be involved in resolving this situation. This event will be evaluated to determine what caused this medical error and to take steps to make sure it doesn’t happen again. (But it will happen again, but usually not to the same patient.)
Ultimately, the doctor will need to sit down and to talk about where to go from here. Since the CPR was performed, what condition is the patient in? What options are available which would be respectful of Mrs. Garcia’s wishes? Is it time for a hospice referral? The doctor who performed the CPR may not be the best person to handle the situation at this point because of the broken trust. It may be necessary to bring in a different consultant to help bring peace to this situation. It will also be important to address Mr. Garcia’s anger and frustration with the hospital and the healthcare team. He will probably be devastated that his wife’s wishes were not honored and that she is still suffering. Appropriate social services should be brought in to help him with his grief.
Upon evaluation of the event, it appears that it wasn’t that Mrs. Garcia’s wishes weren’t respected, but her wishes were not known (because no one read her advance directive) and the CPR/DNR conversation never occurred. This is also a common problem in healthcare. Many physicians are uncomfortable talking about end-of-life issues. I would hope that healthcare professionals don’t just talk about the medical choice of CPR but would also talk about what kind of life one would want after CPR and what kind of death is desired. The following questions are just as important as, “Do you want CPR?”
Where would the person want to die?
Whom would the person want to be with as he or she dies?
What would bring peace and comfort during the dying process?
For many people, CPR just prolongs the dying process, is this okay?
Conclusion:
The conversation about CPR and other end-of-life decisions is a journey of informing, understanding and helping to support the person who has the difficult choice to make. As professionals, we have to find the courage to walk with our patients as they move through their illness and toward death. As patients and family members, it is important to have these conversations early on and I would encourage everyone to ask for the answers and support you need. If the doctor won’t talk to you, find a doctor who will. And if after talking with the doctor, you realize he won’t respect or support the patient’s wishes, find a doctor who will. Once you have made the decision, write it down and tell others what you would want. Don’t make them guess.
A final thought: I am not saying that people shouldn’t choose to attempt CPR; I just want to make sure patients and their loved ones have the facts about what is CPR, the chance of it working, the kind of condition the person might be in after CPR and the kind of death that is being chosen. Make wise and informed decisions for yourself and for those in your care. Have a kind and respectful day.
Study Questions:
What are the common misunderstandings about CPR?
When talking about DNR, what other issues should be discussed?
What do you think would get in the way of you making a good decision for your loved one?
What decision would you make regarding CPR/DNR and how does that affect how you interact with those you serve?
References
Diem, S. J., J. D. Lantos, and J. A. Tulsky. 1996. Cardiopulmonary resuscitation on television: Miracles and misinformation. New England Journal of Medicine 334 (24): 1578–82.
Ehlenbach, W.J., A.E. Barnato, J.R. Curtis, et al. 2009. Epidemiologic
study of hospital cardiopulmonary resuscitation in the elderly.
New England Journal of Medicine 361 (1): 22–31.
Gordon, S. 2009. CPR Survival Rates for Older People Unchanged.
HealthDay: News for Healthier Living, July 1, 2009.
Kaldjian, L.C., Z.D. Erekson, T.H. Haberle, et al. 2009. Code status discussion and goals of care among hospitalized adults. Journal of
Medical Ethics 35 (6): 338–42.
Peberdy, M.A., W. Kaye, J.P. Ornato, et al. 2003. Cardiopulmonary
resuscitation of adults in the hospital: A report of 14,720 cardiac
arrests from the National Registry of Cardiopulmonary Resuscitation.
Resuscitation 58
Have a kind and respectful day.
DNR (do not resuscitate or no CPR) does not mean do not treat or do not care. A warning for all of us.
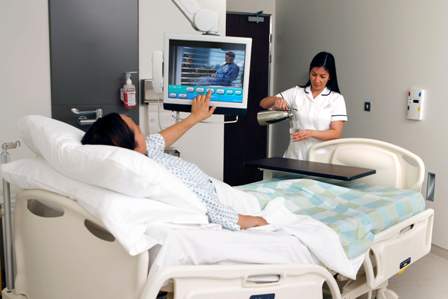
Dear Viki,
I noticed that after my dad became a DNR in the hospital, the nurses didn’t come into the room as often anymore and the doctor didn’t visit the way he used to. Just because my dad didn’t want to have CPR didn’t mean that he still didn’t want to fight his cancer. But it seemed like everybody gave up on him. Did the DNR (do not resuscitate) decision really mean, Do Not Care?
I realize that not only are patients confused about what DNR means (do not do CPR), but nurses and physicians are also confused. I know that’s not what you want to hear, but it’s true. Somehow DNR has become a decision about treatment choices instead of just CPR. What DNR should mean is only one thing, do not do cardiopulmonary resuscitation.
Research has found that if a patient is a DNR, then healthcare professionals may believe that the patient doesn’t want any other types of aggressive treatment. But this isn’t true. A patient may want chemotherapy, surgery, radiation therapy or other kinds of aggressive treatments, and still not want to receive CPR. A DNR doesn’t tell you anything about what other treatments the patient might or might not want to receive.
I’m not telling you this to scare you out of being a DNR. Not at all. I am just reminding all of us that one part of the end-of-life decision making process does not dictate everything else we might want. So yes, you can be a DNR and still have appropriate aggressive medical treatments. Or you can be a DNR and choose only to have hospice care. Or you can be on hospice and not be a DNR. Or you can choose some of the medical treatments being offered and refuse others. These are all separate decisions. You get to choose from all of the appropriate medical options available. Choose some, choose all or choose none. It is up to you. The only thing you can’t choose is a treatment that is not a valid medical option. You cannot make the doctor gave you ineffective or non-beneficial treatments. You are only allowed to choose from the list of medically appropriate treatments for your condition.
Lastly, as a reminder to all the healthcare professionals. A DNR never represents a do not care order. We should still be going into their hospital room as often as we would for someone without a DNR. We should always treat the patient with respect and dignity and provide comfort care to manage their suffering.
Have a kind and respectful day.
Why did the doctor do CPR against the patient’s will?
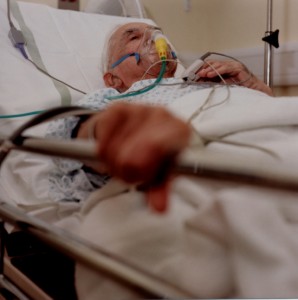
Dear Viki,
I just got the call that my father-in-law was resuscitated (got CPR) twice even though he had a DO NOT resuscitate order in place. Instead of a being allowed to die, now he is in the ICU and receiving care he doesn’t want. What just happened? What do I do next?
Even though this isn’t supposed to ever happen, it happens at all hospitals. A DNR or a do not resuscitate order should be followed but sometimes because people are in a hurry or don’t check the chart or don’t agree with the order, and the person is brought back to life against their will. This is a terrible thing for the patient and family to go through, Instead of the patient getting to die a natural death, they receive medical care against their will.
Here is the truth about this situation. If the medical professionals knew that there was a DNR in place, then what they did to your father-in-law is called assault and battery. The people involved can be arrested and criminally charged. And I need to let any healthcare professionals that might be reading know that your malpractice insurance won’t cover this because it is a criminal offense.
But what can you do now that it has happened. The best thing to do is to talk to the nurse and find out if they realize they made a mistake. (Don’t be hostile or aggressive as these caregivers are still taking care of your father-in-law.) Be polite and make sure that there really is a DNR written on the chart and that they will make sure it is respected. Sometimes we think these instructions have been written but the doctor hasn’t gotten around to it or won’t write it. There are some physicians that are morally opposed to the DNR and are supposed to tell you that they won’t do it. But many times they won’t tell you or even let you know it is a valid medical option. If the doctor won’t write the DNR, then fire that doctor and get another doctor to write it immediately.
You may also want to notify the hospital administrator who is on call. Let them know what has happened and they can help you. The other person that can help you is the social worker. The social worker will know who to call and will help advocate for the patient.
Another note: I spoke with this person directly and found out that the family thought that the patient had a DNR but really only had an advance directive that said do not resuscitate. Those wishes were not transferred onto the chart. This is something we need to be careful about. Just because the patient may have refused a certain treatment, it doesn’t really count until it is known by someone on the healthcare team. Of course the patient’s wishes should always be respected, but these are serious orders about life and death and they must be written out by the doctor. (It still might be assault and battery if the patient’s wishes in the advance directive were known by the healthcare professionals.) Make sure you go over your loved one’s advance directive doctor when you arrive at the hospital.
4th Edition Available – Resource Workbook, Visual Tools and Conversation Guide
November 22, 2014 by Viki Kind
Filed under Featured, For Healthcare Professionals, For Patients & Families
WORKBOOK AVAILABLE ONLY BY CONTACTING VIKI DIRECTLY
I am excited to let you know the 4th edition which has 12 new pages of uniquely designed visual conversation tools is now available. It includes articles, worksheets and templates you can copy and share to help with issues such as evaluating danger, making challenging medical decisions, managing caregiver burnout, and communicating your end-of-life wishes. – Order here or email Viki directly. Resource Workbook, Conversation Guide and Visual Toolkit 135 pages (8½ x 11)
Usually $40 – SPECIAL: $34.95 plus sales tax and shipping
 Table of Contents
Table of Contents
- Section 1: Medical Decision Making Tools
- Crisis Planning Worksheet for Urgent Decision Making
- Quick Tips for Crisis Decision Making
- Drawing an Outcome Roadmap Article and Diagram
- Recovery is Not a Straight Line – Managing Expectations
- Weighing the Options – Risks, Benefits and Burdens
- Weighing the Options Exercise
- Is the Patient Willing to Endure the Burdens to Get the Benefits?
- Double Weighing the Options Exercise
- Combining an Option Roadmap with the Risks, Benefits and Burdens When Discussing the Alternatives Article and Diagram
- Two-Hand Test for Medical Decision Making
- Two-Hand Test for Medical Decisions Making Diagram
- Evaluating Medical Options Through Three Lenses
- Evaluating Medical Options Through Three Lenses Diagram
- Sliding Scale for Acceptability: Where are the Patient’s Boundaries?
- Sliding Scale for Acceptability Exercise
- Evaluating Treatment Options When You Know the Patient’s Long Term Goals Article
- Evaluating Treatment Options When You Know the Patient’s Long Term Goals Algorithm
- Four Boxes Motivation Article and Exercise – Exploring Why thePa tient Isn’t Following Your Treatment Plan
- 5-Step Process to Help the Person Get Out of Denial
- Questions to Ask When Making Medical Decisions
- 6 Tips to Improve Communication with Your Doctor
- Getting Ready for Your Doctor’s Appointment
- Section 2: Evaluating Danger and Risk Tools
- Can the Person Connect the Dots?
- Evaluating Danger and Risk When Making Decisions
- Evaluating Risk for Those Without Capacity Diagram
- Evaluating the Dangers Worksheet
- Solutions to Creating a Restraint-Free Life
- Section 3: Caregiver Conversation and Support Tools
- Are You Care-grieving?
- The Ladder Diagram – The Caregivers Needs Count Too!
- Using the Ladder Diagram
- How is Your Relationship Now That Illness is a Part of Your Lives?
- Viki Kind’s 4-Step Process for Asking For and Accepting Help
- 4-Step Process for Asking For and Accepting Help Worksheet
- Caregivers and Guilt
- How to Say “No” Handout
- Section 4: End-of-Life Conversation Tools
- Insider’s Guide to Filling Out Your Advance Healthcare Directive
- Quick Tips for Filling Out Your Advance Directive
- Quality of Life Statement Template
- Viki’s Quality of Life Statement
- Guidance for My Decision(s) Maker
- What I Want My Doctor to Know About My Faith and/or Culture
- Having My Doctor Review My Advance Directive
- 5 Quick Tips for Making the CPR vs. DNR Decision
- Avoiding the Pitfalls in CPR vs. DNR Decision Making
- Recommended Books and Additional Resources
- Acknowledgements
Clarifying How to Use the Structure of my new Quality-of-Life Statement to Make it Your Own
March 22, 2013 by Viki Kind
Filed under For Healthcare Professionals, For Patients & Families
The goal of writing a quality-of-life statement is to have it express your personal preferences and to have it sound like you. One of the problems with many of the legal/medical forms is that they all sound alike and they don’t allow your voice to be heard. I encourage you to use the categories I have listed below to express what you would want people to know about you if you were too sick to speak for yourself. You can use some of my language from my document at http://kindethics.com/2012/01/my-new-quality-of-life-statement-to-attach-to-my-advance-directive/ if you would like but my goal is for you to make it personal and meaningful to you. You will know you have gotten it right if people say to you, “Yes, this is sounds like what he/she would say.” By making it feel personal, you will help your family/friends feel more confident that they are truly honoring your wishes.
Sections of QOL Statement to Consider Including in Your Directive:
? Types of illnesses where this advance directive would apply.
? What is important to me?
? What conditions would I find reprehensible to live with long term?
? CPR, ventilator and feeding tube preferences.
? Reassurances for the decision maker.
? What is a good death in my opinion?
? What I want the doctors know about honoring my religious/cultural beliefs both while I am sick and/or dying?
If you have questions, feel free to contact me at kindethics@gmail.com. If you would like to share your new document with me, I would love to see it so I can see how the structure is working.
Have a kind and respectful day.
My New Quality-of-Life Statement to Attach to My Advance Directive
January 3, 2012 by Viki Kind
Filed under Featured, For Healthcare Professionals, For Patients & Families
The goal of writing a quality-of-life statement is to have it express your personal preferences and to have it sound like you. One of the problems with many of the legal/medical forms is that they all sound alike and they don’t allow your voice to be heard. I encourage you to use the categories I have listed below to express what you would want people to know about you if you were too sick to speak for yourself. You can use some of my language from my document below if you would like but my goal is for you to make it personal and meaningful to you. You will know you have gotten it right if people say to you, “Yes, this is sounds like what he/she would say.” By making it feel personal, you will help your family/friends feel more confident that they are truly honoring your wishes.
Sections of QOL Statement to Consider Including in Your Directive:
? Types of illnesses where this advance directive would apply.
? What is important to me?
? What conditions would I find reprehensible to live with long term?
? CPR, ventilator and feeding tube preferences.
? Reassurances for the decision maker.
? What is a good death in my opinion?
? What I want the doctors know about honoring my religious/cultural beliefs both while I am sick and/or dying?

Here is my new quality-of-life or meaningful recovery statement. My wishes haven’t changed but how I am saying it is much more complete. Feel free to take any part of it you would like. Use the basic headings and then make it personal and meaningful for you. I would recommend attaching it as an addendum to a basic advance directive form that works in your state.
Advance Healthcare Directive for Viki Kind – dated 11/1/2012
Types of illnesses where this advance directive would apply whether I am terminal or not terminal.
I can never list every type of disease that might make me begin to lose my mental capacity but the list might include, but not be limited to: all types of dementias, stroke, brain injury, mental illness, anoxic event, etc. I don’t have to be completely out of it like being in a coma, persistent vegetative state, or minimally conscious state for this document to go into affect. And I don’t have to be terminal. The point is that I don’t want to have my life prolonged/sustained if my brain no longer works well enough to enjoy what is important to me.
What is important to me? (The loss of any of these might be enough for my decision maker to implement my wishes documented in this advance directive.)
To make a difference in the world.
To be able to communicate with those I love.
To receive the joy that comes from personal relationships.
To have some independence.
To be able to give love, not just receive people’s kindness.
To not be a burden on my family/friends – financially, emotionally or physically.
To have a good death as defined by me (see below).
What conditions would I find reprehensible to live with long term? (Please give me the chance to recover if recovery is possible, but if I am not recovering to a level of functioning that I would think is worthwhile, whether terminal or not, then choose comfort care and hospice which I understand will lead to my death.)
All of the following conditions do not have to be present at the same time for the decision to be made to allow me to die from my illness/injury. Any one of these conditions may be sufficient enough to change my course of treatment from prolonging my life to comfort care and allowing a natural death.
This list of “Conditions I would not want to live with” includes but is not limited to:
Not recognizing my loved ones.
Not being able to communicate by voice, computer or sign language.
Wandering around aimlessly.
Suffering that isn’t necessarily pain related.
Significant pain that can not be controlled.
Significant pain that requires so much medicine that I am sleeping all the time.
Having to live in a skilled nursing facility or sub-acute facility permanently with my cognitive impairment. Nursing homes create such sadness in me every time have I visited or have stayed overnight with a loved one. I am too empathetic and take in people’s suffering too easily to be in that environment. It would destroy me long term. A short-term stay in a SNF/rehab/sub-acute is okay if I can recover to a life that I would consider worth living. (I understand that with certain types of traumatic brain injuries, they take a longer period of time to evaluate whether or not recovery is possible.) But if it looks like I am not recovering, then no thank you.
Okay, now the CPR, ventilator and feeding tube conversation.
My overall guideline is that if CPR, ventilator support or a feeding tube/TPN can return me to what I would consider to be a meaningful existence, (what is important to me), then please give me CPR, ventilator support and/or a feeding tube/TPN. But there has to be value in these medical options and any other medical treatment choices that are being considered. Don’t do things, including but not limited to, antibiotics, etc., that are just to sustain my poor condition.
I am not opposed to living with a feeding tube/TPN if it gives me many years of being able to enjoy what is important to me. But if the feeding tube/TPN is just to sustain my miserable condition, (what I would consider reprehensible) then don’t put it in or give me feedings through it; and please take the feeding tube out if it is already in. (Okay, if I am on hospice and the feeding tube gives you access for administering the pain and suffering meds I need, then you can leave it in. But don’t put food or additional liquids in it.) The feeding tube, like all medical decisions, needs to create value in my life, not just sustain my life.
If I am still healthy and can still experience lots of the things that are important to me, then give me CPR. But as my health declines and CPR becomes less statistically successful, then make me a DNR. Just like many doctors, I don’t want to die by CPR. I want to die peacefully without life-prolonging medical interventions. (Doctor, please ask yourself the surprise question: Would I be surprised if Viki died during this hospitalization or died in the next 6 months? If the answer is “No, I wouldn’t be surprised,” then talk to my decision maker about end-of-life choices, including putting me on hospice.)
Reassurances for the decision maker
You are allowed to make the best decisions you can based on the circumstances and what you know at the time. You do not need to know for certain or absolutely that you have all the answers. The decision doesn’t have to be perfect. Use your heart and your head. I trust you to do the best you can. (Ed, you don’t have to go into super-perfectionist mode.)
I believe love does not obligate a person to sacrifice themselves to be the caregiver for another. The damage done to the caregiver, emotionally, physically and mentally is too costly. I do not expect someone to give up their mental, emotional and physical health for me. Look at the MetLife studies. Caregiving sucks. And I love my decision maker and alternates too much to impose such a burden on them.
(Ed, if you need some time to make peace with what has happened, then you can take the time you need. I don’t want the decision to feel rushed or uninformed, which would cause you a lifetime of regret.)
For you doctor, your role is to give my decision maker as much information as you can so he/she can make an informed decision. I encourage you to share your wisdom, guidance and experience but ultimately, it is my decision as expressed through my decision maker and this document. Remember, this document is an act of autonomy and should not be ignored by my decision maker/s, other family members, doctors or worst case, the courts. (I will definitely come back and haunt a judge who isn’t respecting my wishes.)
What is a good death in my opinion?
I would prefer to die at home but I realize that sometimes, a person needs to die somewhere else so I accept that. I would like to have my family/friends with me which includes and is limited to those I interact with on a regular basis. Those family/friends who have chosen to not be in my life while I was living should certainly not be there as I am dying. Because I like control over my life, I would like to be able to clean up my desk and to get my financial information updated. I would like to be able to write love letters, record messages and to say my goodbyes. (I will do my Go Wish Cards and leave a copy for my family.)
I would like to die with reasonable pain control. For the days leading up to the death, I would be willing to tolerate a certain amount of pain if that allowed me to have meaningful time with family/friends. But at the end, there had better be no pain and definitely, no air hunger. (That doesn’t mean ventilator support; it means manage my air hunger with medications.)
And you better not be force feeding me by mouth, by IV or by tube as that would increase my suffering. (And that includes you at the skilled nursing facility, sub-acute facility or other care community if I happen to be dying there. I know you have your regulations but I also know you can’t assault someone with food if they have said no when they had capacity.)
That’s it for now.
Viki Kind ________________________________
Date: 11/1/12
Coalition for Compassionate Care – Building a Community of Caring – CCCC 3rd Annual Conference on March 16 from 8-4:45
March 7, 2011 by Viki Kind
Filed under Uncategorized
Coalition for Compassionate Care – Building a Community of Caring – CCCC 3rd Annual Conference
Where:
Los Angeles Marriott Hotel Burbank Airport
2500 Hollywood Way
Burbank, CA 91505
When:
Wednesday March 16, 2011 from 8:00 AM to 4:45 PM PDT
Join doctors, nurses, social workers, administrators and lawyers from around the state to discuss the latest cutting-edge issues in end-of-life care. Learn the latest advancements in end-of-life care, connect with others in your profession, see the newest available resources, and expand your understanding of compassionate care.
Speakers include:
David Kessler, a well-known expert on hospice, dying and grieving, talking about his latest book, Visions, Trips, and Crowded Rooms: Who and What You See Before You Die.
Joanne Lynn, MD, MA, MS, one of the first hospice physicians in the US and a major contributor to research and policy on care for the last phase of life, discussing how to build a local end-of-life community.
Mary Cadogan, DrPH, RN, NP, a gerontological nurse practitioner and professor at UCLA School of Nursing, outlining the latest research on CPR.
LaVera Crawley, MD, MPH, Assistant Professor at the Stanford University Center for Biomedical Ethics, examining culturally sensitive end-of-life choices.
Plus three California authors who have recently published books on end-of-life care. (Viki is one of the featured authors.)
Pre-Conference Workshop
Building Bridges: Culture and End-of-Life Care
Tuesday, March 15, 2011
Lunch & Registration: 11:30am
Program: 12:00pm – 4:30pm
Have a kind and respectful day.
Taking Action to Solve the Healthcare Conflict
November 23, 2009 by Viki Kind
Filed under Newsletter

Quote of the day by William James: “Whenever you’re in conflict with someone, there is one factor that can make the difference between damaging your relationship and deepening it. That factor is attitude.”
Taking Action to Solve the Healthcare Conflict
It doesn’t matter who is the problem or who is at fault. You have to take action now to get the conflict resolved and to move forward taking care of your loved one. If you have been part of the problem, say you’re sorry. If you aren’t the problem, don’t worry about getting an apology. You don’t have time to stay angry. Your loved one needs help. The first thing you want to do is to deal with any conflicts when they first arise instead of letting them escalate. There are problem solvers throughout the hospital: The social worker, the charge nurse, the chaplain, the bioethics committee, the hospital administrator and in some places an ombudsman. These people have been trained to help facilitate the conflicts that occur in the hospital. If the conflict is happening in the doctor’s office, then you are on your own. But don’t worry, after you read the next few pages, you will be a much better problem solver yourself.
The first thing you need to do is to look at your role in the conflict. Am I making this situation better or worse? What could I do to make this situation better? Is this how I would react on a normal day? Or am I just overwhelmed, afraid, in shock or in grief and I’m having a hard time coping with this situation? Sometimes we need to take a timeout to catch our breath before we can interact with others and make any meaningful decisions. It is normal for you to feel the pressures and weight of these decisions. When any of us are in a crisis, we are not at our best. But unfortunately, you may not have the time to process what you’re going through and be able to feel like yourself again. Sometimes we have to make the decisions while we are stressed. Let people know how hard this is for you so they will understand what you are going through.
A couple of questions, you can ask yourself, may help you begin to see the situation differently. Are you making inaccurate assumptions? Sometimes we have misunderstood or not heard correctly what has been said to us. Before you get upset, make sure that you have the right information.
Are you more interested in “being right” or “getting it right”? This is a tough one. If you are determined that your way is the only way you, then you are going to have a difficult time resolving the conflicts with the healthcare team. Too often people discover that the way they thought things should go, turns out to be a mistake. I have seen this many times when the bioethics committee comes in to help with the ethical dilemma. The doctor is determined that his way is the right way and he is frustrated that the patient will not agree. Or the patient’s loved one comes in ready to do battle. Here’s what happens. As the meeting goes on, the people in the room hear the other parts of the story that they didn’t know before. Perhaps the doctor finds out that the reason the patient doesn’t want to do the surgery is because there’s no one at home to take care of them. The patient isn’t trying to be difficult, they are just feeling helpless. Or the patient’s family finds out that they have misunderstood what the doctors said about the disease or the possibilities of a cure. Once the misunderstandings have been cleared up, people calm down and new decisions can be made.
You have a lot of power in all of these interactions. You have the power to escalate or de-escalate the anger. You might say something like, “That’s the stupidest thing I’ve ever heard.” Well you can say this but it is only going to make the other person angry and you will still be no closer to getting what your loved one needs. Instead you might want to try a different approach. You might want to say, “Let me see if I understand what you are saying.” Or, “It seems like we both are trying to achieve the same thing but in different ways. Maybe if we …” If you think there is some miscommunication going on you can say, “I heard what you said. Let me repeat it back to you to see if I have understood you correctly.”
When I tell people this idea, people will say to me, “I don’t like what they are saying and I don’t agree with what they are saying.” Of course you don’t agree. You are in a conflict. But I never said you should agree. All I said was that you should listen to their point of view. This is the secret that mediators use to solve dilemmas all the time. One of the main things a mediator does is to help the people in the room to stop and listen to each other. You are listening to figure out if there is new information you didn’t hear before, or if there is some kind of misunderstanding or if you can understand more about why the other person is so passionate about their point of view.
This is where your power is in the middle of the conflict. It is not in raising your voice or pushing for everyone to do it your way. The power comes from understanding what is really going on and hearing what the other person needs you to know about what this means to them. I will never say that to listen means to agree; not at all. It just means to listen.
When you listen to resolve a conflict, the anger and emotions will decrease and your empathy will increase. You may surprise yourself when you finally hear what they are really saying because you may find yourself feeling more compassionate and understanding of their position. You will know that the listening is working when the other person begins to calm down. The more you listen, the more you will be able to hear the deeper message behind the other person’s words. Unless you have a really bad person in the room, you need to remember that the people helping your loved one want your loved one to get better too. (If there is someone who is really bad on the healthcare team, why are you keeping them on your team? You are allowed to change who is caring for you in a hospital. You can always ask for a different doctor to be your doctor.)
You are probably not disagreeing about the goal of getting your loved one better; you are probably just disagreeing on the how. Give the person you are arguing with the benefit of the doubt and stop and listen to what they have to offer. You may like what you hear. (I have seen in many bioethics meetings that people will completely change their minds and agree with the other side once they understand what is really going on.)
You won’t be able to solve the problem until you understand the interests behind the position. What does this mean? It means that what the person is saying he wants is only part of the issue. The trick is to figure out what the demand really represents. Let me give you an example. The loved one is demanding that the patient get CPR. The doctor wants the patient to be made a DNR (Do Not Resuscitate). Now there is a conflict.
If I was helping these two to solve their conflict, I would first listen to try to figure out why it is so important to them to have their way. I would ask the patient’s loved one, “Why it is so important to have the patient get CPR?” They may tell me that they are desperate for the person to recover so they can ask for forgiveness. They haven’t been a good son and they want to say I’m sorry. Or they might say that it is against the patient’s religion to be a DNR. Or they might tell me that the patient said he would want CPR and they are trying to honor his wishes.
Do you begin to see now why what they want matters? If I can figure out why they want ____, then I can figure out how to help them. (And I figure this out by listening.) The same thing goes for the doctor. Why does the doctor want the patient to be DNR? Well perhaps the patient is close to dying and the doctor knows CPR won’t work. Or the doctor doesn’t want to prolong the suffering of the patient. Or the doctor doesn’t want to lose the business. Again, do you see why the why matters?
This is the power of listening. You can discover what is really going on behind the person’s demands and begin to figure out a way to solve it together. When you are listening, focus on figuring out what you have in common. Are you both trying to get the patient better? Are you both trying to respect the patient’s wishes? Anything you can find in common will become a starting place for problem solving.
I would like to give you a couple of quick tips to help you problem solve. The first is to separate the person from the problem. How do we do this? In these situations, it becomes a conflict between “my way” and “your way”. And we just keep battling until either one of us wins or we both get more frustrated. This doesn’t do the patient any good and it wastes our time. Let me give you an example. The patient comes in and he hasn’t been taking his medication. Usually the doctor would say, “Why haven’t you been taking your medication?” And what the doctor really means is, “Why are you being a problem?” This approach rarely works. So, instead you might want to say to the patient, “How are you and I going to solve the problem of the medicine getting into you?” The problem becomes the third person in the room. You have separated the person from the problem. Now the patient isn’t the problem, the problem is the problem. This takes the pressure off the situation and the two of you can begin to brainstorm to figure out a workable solution.
One quick note before you start brainstorming, make sure you remember to understand what the real issue is before you start. It is a waste of your time to work on solving the wrong problem. Is the patient not taking his medicine because he can’t afford it? Is he not taking his medicine because he doesn’t like the way it makes him feel? Or is he not able to cut the pill in half or open the medicine bottle? These are just a few examples of the many reasons a patient might not be taking the medications. Figure out what the real issue is and you’ll be able to solve the problem together.
The second tip is to use brainstorming to come up with more options. Brainstorming is when everyone comes up with new ideas on how to solve the problem. One technique which mediators use is to make sure the people in the conflict come up with at least three alternatives. This begins to break the conflict right away. It is no longer my way versus your way. As you begin, you can start with my way, your way or do nothing then work from there. You will find that the more options you can think of, the more likely you will be able to find a solution that people can live with. As you continue to brainstorm, you might realize that you could do a little bit of what you want and a little bit of what they want. Or you could throw out both of your plans and start again. Not only does brainstorming create a safe place to come up with new options but because you two are doing it together, it will change the experience from a combative process into a collaborative process.
Another you might want to do is to take a “time-out”. Not only does it help people calm down but in it also allows people to think about what has been discussed and to process what they have learned about the situation. We have all heard the phrase, “I have to sleep on it.” Sometimes we have to have patience and allow the other person some time to think. If you try to push someone who is not ready into making a decision, you may get a decision but it probably won’t last. The person will come back the next day and say, “I changed my mind.” I am not surprised when this happens because the person wasn’t ready to decide in the first place. Also, in some cultures, people need to go home and talk with their family or religious and community advisors. Allow people the space and time to make good decisions.
The most important part of this process is to work together. If you stay in a battle mode, you will continue to battle. When you stay in the war, the patient loses. Take responsibility for your part and make the effort to fix the situation. Be willing to say, “I was wrong. Or, I didn’t understand.” Realize that you can disagree without being disrespectful and hurtful. Figure out how you can invite this person into the problem solving process with you, especially during healthcare conflicts. You are still going to have to deal with this doctor or person on the healthcare team tomorrow. So it is better to peacefully resolve the issues than to create a battleground. Take the time to listen so you can begin to understand and empathize with the other person. You have the power to turn the conflict into an opportunity for things to get better.
Have a kind and respectful day.
Definitions
April 5, 2009 by Viki Kind
Filed under
Advance Directive – This is a written document that says what types of medical treatment you desire and who the doctor should talk to when you are unable to speak for yourself. This document is also considered to be a combination of a Living Will and the Durable Power of Attorney for Healthcare.
Agent – This is who the doctor should talk to when you are unable to speak for yourself. Other terms would include: Power of Attorney for Healthcare, Proxy or Surrogate Decision Maker.
“AND” – AND or Allow Natural Death is another way to say DNR. AND is a request to not have cardiopulmonary resuscitation (CPR) if your heart stops or if you stop breathing.
Autonomy – Autonomy means that a person, with decisional capacity, is allowed to make their own decisions about what will happen to their body.
Beneficence – Healthcare professionals are supposed to do things which will benefit the patient. This concept of balancing the benefits and the burdens or risks should be considered when deciding what should be done.
Best Interest Standard – This standard applies when the patient doesn’t have any loved ones to speak for them or the patient can not speak for themselves and express their wishes. We make decisions the best we can for this unknown patient.
Capacity – This is when the patient has the mental ability to make their own decisions.
Compentent or Competency – This is a legal term to describe when a person has the ability to make their own decisions.
Conservator – This is a court appointed person who is assigned to make decisions for an incapacitated person. This term is similar to guardian in most states. They may be in charge of medical decisions, financial decisions or both.
“CPR” – Cardio Pulmonary Resuscitation which is attempted if your heart stops or if you stop breathing.
Decisional Capacity – This is when the patient has the mental ability to make their own decisions.
“DNAR” – DNAR is another way of saying DNR. DNAR means DO Not Attempt Resuscitation and is a request to not have cardiopulmonary resuscitation (CPR) if your heart stops or if you stop breathing.
“DNR” – DNR stands for Do Not Resuscitate. A DNR is a request to not have cardiopulmonary resuscitation (CPR) if your heart stops or if you stop breathing.
Durable Power of Attorney for Finances – This is a written document that says who should be in charge of your money when you are unable to make your own decisions. This document does not include medical decision making power.
Durable Power of Attorney for Healthcare – This is a written document that says who to when you are unable to speak for yourself.
Fidelity – Acting in someone else’s best interest. Physicians and surrogate decision makers are supposed to do the right thing for the patient even if it isn’t in their own best interest.
Fluctuating Capacity – This is when the patient sometimes has the mental ability to make their own decisions and sometimes no.
Guardian – This is a court appointed person who is assigned to make decisions for an incapacitated person. This term is similar to conservator in most states. They may be in charge of medical decisions, financial decisions or both.
Living Will – This is a written document that says what types of medical treatment are desired. A living will can be very specific or very general. This document could also be called an Advance Directive.
Non-maleficence – The Latin term “primum non nocere” means “do no harm.” What this means is that the physician is supposed to avoid doing things which will cause any unnecessary harm. The concept of balancing the benefits and the burdens should be considered when deciding what should be done.
Power of Attorney for Healthcare – This is who the doctor should talk to when you are unable to speak for yourself. Other terms would include: Agent, Proxy or Surrogate Decision Maker.
Proxy – This is who the doctor should talk to when you are unable to speak for yourself. Other terms would include: Power of Attorney for Healthcare, Agent or Surrogate Decision Maker.
Substituted Judgment – This is when someone else such as a family member or a loved one, makes the medical decisions for a patient who is unable to make their own decisions using the values and wishes of the patient.
Surrogate Decision Maker – This is who the doctor should talk to when you are unable to speak for yourself. Other terms would include: Power of Attorney for Healthcare, Proxy or Agent.
Unbefriended – This term is used to describe someone who doesn’t have any friends or loved ones in their lives that the doctor can talk to when the patient is unable to speak for themselves.
Unrepresented – This term is used to describe someone who doesn’t have any friends or loved ones in their lives that the doctor can talk to when the patient is unable to speak for themselves.
Veracity – Truthfulness, telling the truth.
Keynote/Presentations – for Professionals and Family Caregivers
March 5, 2009 by Viki Kind
Filed under
Evaluating Danger, Risk and Safety when Creating a Care Plan
It is difficult to know when to step in and protect versus stepping back and allowing people to be in charge of their own decisions. The field of bioethics provides families and professionals with a structure and guideline for these managing these situations. Attendees will learn the questions to ask when evaluating the dangers and how to get past not wanting to see the changes that are happening. By balancing the person’s quality of life with the dangers in living that life, families and professionals can feel more confident that they are treating the person with dignity and respect.
Getting Better at Asking For and Accepting Help – for the family caregiver
This course helps caregivers learn how to get past their resistance to asking for help and gives them a 4-step process to help them get the support they need. This is an interactive course where the caregiver will create an action plan that they can use right away. This course will also teach the professional how to use this 4-step process with their clients.
When Caring Hurts – Helping You Get the Support You Need – for the professional caregiver Discuss how professional compassion fatigue may be affecting our interactions. Learn how to say, “No” when people are asking for too much and when to say, “Yes” to taking time for yourself. Demonstrate stress reduction activities.
Identify how build a support system for yourself and within your profession.
Why the Healthcare Directive You Wrote Might Not Work in the Hospital: A Bioethical Perspective and Toolkit
As a bioethicist, I often get called in when the patient has an advance directive that isn’t being honored by the family and/or physician. Learn how to create a personalized quality-of-life statement, to include with the advance directive, to enhance medically appropriate and compassionate healthcare decisions. Discuss how to encourage the patient and family to make meaningful end-of-life decisions while spending money on what really matters
Empowering Caregivers Who Are Facing Difficult Decisions
Wouldn’t it be a relief to know you are making the right decisions and doing right by the person in your care? Whether you are caring for someone with a brain injury, dementia, mental illness, or other cognitive impairment, you can learn the framework and four tools to use when making the difficult life, health and end-of-life decisions. This is not a one-size-fits-all solution but can be adapted depending on a person’s level of incapacity and the situation. Respect and compassion are the core values of this decision making process.
Navigating Healthcare Decisions for Yourself and Those in Your Care
Talking to the healthcare team can seem like we are speaking two different languages. Attendees will learn easy to use communication techniques to help navigate the difficult decisions that caregivers face. When caregivers know the right questions to ask and how to listen to what the doctor is really saying, they can make better decisions about their own health and those in their care.
End-of-life Decisions: A Safe Place to Get Your Questions Answered
End-of-life decisions are difficult enough, but when you combine the loss of mental capacity, it becomes heart wrenching and an ethical challenge. When caregivers know what to expect, these decisions become less scary and overwhelming. Attendees will learn specific questions to ask and strategies to use to make person-centered decisions about CPR, feeding tubes and other end-of-life choices. Caregiver will feel confident and comforted that they did the right thing for the person in their care.
Professional Ethics: The Practitioner’s Obligations and Strategies for Success
4 Ethical Viewpoints – Which One is Right?
Having Moral Courage in Challenging Situations
Who are the Stakeholders and What are Our Obligations to Them?
Principles and Strategies for Situations Involving Fairness and Truth Telling
Simple Tests to Determine “What’s the Right Thing to Do?”
Managing Highly Emotional Conversations
Discuss how to manage the anger, fear, denial and other emotions found in emotionally charged interactions. Identify approaches to change the negative interaction into a more positive, empathetic interaction. Attendees will also practice mediation techniques to reduce conflicts and to increase compassion and respect.
Facilitating Difficult Conversations – Getting Through the Barriers (for the professional)
It would be so much easier if people just listened to our advice and then took action. But there are so many obstacles that stand in the way. Attendees will understand what is motivating non-compliant patients in order to help them get past their personal barriers. They will learn how to deal with the denial and other emotions which interfere with good decision making. Viki will demonstrate person-centered communication strategies and techniques.


